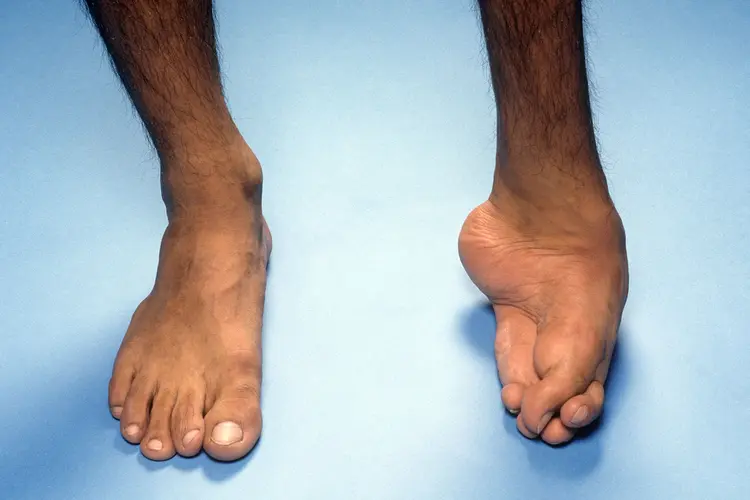
Helping Your Child Stay Active Despite Joint Concerns
Helping your child stay active despite joint concerns like Osteochondritis Dissecans (OCD) begins with understanding the condition and giving your family the tools to navigate it with confidence. Children and teens involved in sports may develop this condition when a piece of cartilage and underlying bone separates from a joint surface, most often in the knee but also in the elbow or ankle. This can cause pain, swelling, and difficulty with movement that may impact participation in play and athletic activities. If you notice persistent joint pain, swelling, or changes in how your child moves, reach out to POBAR to learn how we can help your child stay engaged in life and play. Children who love sports and play may show subtle changes before more obvious symptoms of Osteochondritis Dissecans appear, and those early signs are often the key to preserving joint health while keeping your child active. The discomfort they experience during running, jumping, or pivoting might lead them to stop participating or limp when they walk — signals that merit attention from a pediatric orthopedic specialist trained in OCD care. Rather than simply signaling the end of activity, these early changes offer an opportunity to adjust your child’s routine in ways that protect their joints and still allow for fun and growth. With the right plan, most children can continue to enjoy age‑appropriate movement, even if that looks different from their initial sports schedule. Understanding Osteochondritis Dissecans in Children Osteochondritis Dissecans in children is a joint condition where a fragment of bone with its overlying cartilage becomes weakened and may detach due to interrupted blood supply and repetitive stress on a joint during growth. The knee is the most commonly affected joint, but the elbow and ankle are also susceptible, particularly in young athletes who engage in repetitive motions and high‑impact activities. Symptoms often include pain during activity, swelling around the joint, and sometimes a sense that the joint is catching or locking, which can understandably lead to frustration in an active child. The severity of symptoms and how they affect your child’s daily activities depends on how large the lesion is and whether the affected piece of bone and cartilage remains stable. Diagnosis typically involves a pediatric orthopedic evaluation that includes a physical exam and imaging studies such as X‑rays, which help visualize the bone and joint. In many cases, an MRI is also used to assess how the cartilage and subchondral bone are involved and whether any loose pieces are present within the joint space. These studies give specialists a clear picture of your child’s joint health and help guide individualized treatment plans. What Causes Osteochondritis Dissecans? While the precise cause of OCD remains partly unknown, most experts agree it is linked to repetitive stress or microtrauma to the joint during periods of rapid growth. Young athletes who participate in activities that involve frequent running, jumping, or throwing may be particularly at risk. There may also be a genetic component or variations in joint development that influence how susceptible a child is to this condition. Additionally, periods of rapid skeletal growth during childhood and adolescence may make certain joints more vulnerable to disruptions in blood flow that predispose to an OCD lesion. Although these risk factors can increase the likelihood of an OCD lesion, many children with joint symptoms experience only mild changes that respond well to careful activity modification and monitoring rather than immediate surgery. Understanding these factors can empower parents to make thoughtful decisions about activity levels and rest. Recognizing Symptoms That May Affect Activity Children with Osteochondritis Dissecans may exhibit several symptoms that can interfere with normal play and sports participation: Pain with Activity: The most common sign is discomfort that increases with weight‑bearing activity and may improve with rest. Swelling and Tenderness: Some children experience noticeable swelling around the affected joint after exercise or prolonged use. Decreased Range of Motion: Your child might have difficulty fully bending or straightening the knee, elbow, or ankle. Catching or Locking: Sensations of the joint locking or catching during movement suggest that a fragment may be interfering with smooth motion. Instability: A feeling that the joint is “giving way” can make your child hesitant to participate in activities that require sudden changes in direction. These symptoms often prompt families to reduce activity to avoid pain. However, the goal is to find a balance that protects the joint without completely isolating your child from movement, which is essential for overall health and wellbeing. How to Help Your Child Stay Active Safely Supporting your child’s desire to stay active while managing Osteochondritis Dissecans involves strategic adjustments that protect the affected joint and promote healing: Activity Modification: Instead of high‑impact sports, encourage low‑impact activities like swimming or cycling, which strengthen muscles without excessive stress on the joints. Proper Warm‑Up and Cool‑Down: Ensuring your child warms up before play and cools down afterward can reduce joint stress and help maintain flexibility. Strength and Flexibility Exercises: Physical therapy focused on strengthening the muscles around the joint can improve stability and support healthy movement. Structured Rest: Incorporating rest periods into your child’s routine helps reduce inflammation and gives injured cartilage and bone a chance to recover. Protective Gear: Using braces or supportive padding during high‑risk activities may provide additional joint support without completely stopping activity. These approaches emphasize keeping your child engaged in movement that feels good and is appropriate for their stage of healing, rather than eliminating activity entirely. Your pediatric orthopedic specialist can help you tailor these strategies based on your child’s symptoms and lifestyle. When to Consider Specialist Intervention If your child’s symptoms persist despite activity modification and supportive care, or if imaging studies show a loose fragment of bone within the joint, our pediatric orthopedic specialist may recommend more structured interventions. In growing children, many OCD lesions can heal with conservative approaches like rest, temporary immobilization, and gradual return to activity under guidance. However, if the lesion doesn’t heal or pain continues, surgical options such as drilling